Last updated: May 2026
The Herbst appliance has been the workhorse of fixed Class II correction for more than a century. It works. It also breaks. Historical complication rates reached as high as 88% in older banded designs. Modern designs cut that significantly. The prescription decision is not “Herbst yes or no.” It is which Herbst design fits this case, this patient, this hygiene reality.
We fabricate Herbst appliances for orthodontists across the country and invented the MiniScope® Herbst over two decades ago to address some of the cons listed below. This article reads the trade-offs by design parameter, with the published complication data and lab-side observations as the anchor.
Is the Herbst Worth Prescribing?
The Herbst appliance is worth prescribing for Class II malocclusion correction in growing patients near the pubertal growth peak, when 24/7 fixed-appliance compliance is preferable to removable-appliance wear enforcement. The main trade-offs are design-dependent breakage rates (roughly 20% in modern designs, historically up to 88% in older banded configurations), post-treatment relapse risk, and hygiene burden during active treatment.
The Pros: What the Herbst Does Well
The case for the Herbst is clinical, not promotional.
Compliance is built in. The Herbst is fixed. Once placed, it works 24 hours a day without patient enforcement. The clinician does not need to police wear time. For adolescent patients, this is often the deciding factor over twin-block, bionator, or similar removable functional appliances where compliance determines outcome.
The outcome literature is mature. Hans Pancherz published continuously on the Herbst from 1979 until his death in March 2023, including long-term follow-up studies of treated patients beyond 30 years post-treatment. The clinical effects (skeletal mandibular response in growing patients, dental compensation in non-growing patients, the “headgear effect” on the maxilla) are well-quantified. Pancherz’s 1982 AJODO mechanism paper documented 6.7 mm of Class II molar correction across 42 cases, broken down to approximately 2.2 mm mandibular length increase, 2.8 mm distal maxillary molar movement, and 1.0 mm mesial mandibular dentition shift. Few orthodontic appliances have this depth of published evidence.
Treatment time is predictable. Active Herbst phase typically runs 6 to 12 months depending on Class II severity, with multibracket finishing following. The fixed appliance, continuous activation, and 24/7 wear produce a predictable timeline that the clinician can build into the treatment plan.
Skeletal contribution in growing patients is real. In patients near or just after the pubertal growth peak, Herbst treatment produces measurable mandibular growth response, not just dental tipping. This separates the Herbst from purely tooth-borne Class II correction options.
The Cons: What the Herbst Gets Wrong
The case against the Herbst is also clinical.
Breakage and emergency visits. Older banded Herbst designs reported complication rates as high as 88% in some published cohorts, with emergency visits driven by appliance breakage, attachment loosening, telescope rod fracture, and cementation failure. Even modern designs have non-zero complication rates. The clinician should expect chairside repair visits during the active treatment phase.
Hygiene burden. The telescoping mechanism, attachment hardware, and crowns or bands create plaque retention zones the patient must clean diligently. Adolescents do not always clean diligently. White spot lesions, gingivitis, and decalcification around Herbst hardware are documented complications.
Soft tissue irritation. The buccal corridor placement of the telescoping arms can produce ulcerative lesions of the mucosa, particularly during the adaptation period and in patients with smaller mouths. The literature on the conventional rod-and-tube Herbst documents this consistently.
Post-treatment relapse. This is the under-discussed con. Class II correction achieved with the Herbst is partly skeletal and partly dental in growing patients, and almost entirely dental in non-growing patients. The dental component is prone to relapse without effective retention, and Pancherz’s own long-term follow-up work documented some skeletal and dental relapse over time. Retention planning matters more for Herbst cases than the breakage rate matters for daily practice.
Reduced applicability in adults. While Herbst-in-adults treatment is well-documented (Ruf and Pancherz 2006 reported successful outcomes in 23 consecutive adult cases with pretreatment ages from 15.7 to 44.4 years), the skeletal contribution diminishes significantly past the growth peak. Adult Herbst cases rely more heavily on dentoalveolar effect, which is less stable long-term.
Design-Driven Complication Rates: What the Data Show
The historical 88% complication rate that appears in patient-facing pros/cons articles is misleading without context. It comes from older banded Herbst designs and a broad definition of complication that includes minor reversible events. Modern designs report substantially lower rates with the same definition.
The Manni telescopic Herbst (MTH) versus conventional rod-and-tube (RMS) comparison published in 2014 (PMC8191925) is informative. Across 89 MTH cases and 90 RMS cases:
- The MTH design showed reversible complication rates of 20.2%.
- The RMS design showed reversible complication rates of 51.1%.
- Irreversible complications (requiring appliance removal and remake) did not differ significantly between the two designs.
- The pattern of complications differed: in the RMS group, irreversible complications were typically preceded by reversible ones; in the MTH group, irreversible complications often occurred without prior warning.
The Knösel et al. 2015 study (PMC4564960) on a WIN-Herbst combined with lingual appliance reported 13 complications across 35 patients over the observation period, with 88% of treatments complication-free for 100 days, 70% for 200 days, and 56.8% for 300 days. The complication-free interval for severe complications averaged 27.8 months.
The design parameters that affect complication rate include:
- Anchorage type (banded vs crown-mounted; crown-mounted is generally more durable)
- Telescoping mechanism size (smaller mechanisms produce less soft-tissue irritation but can have different fracture profiles)
- Attachment method (cement, welded, integrated crown)
- Whether splints or archwire anchorage carry primary load
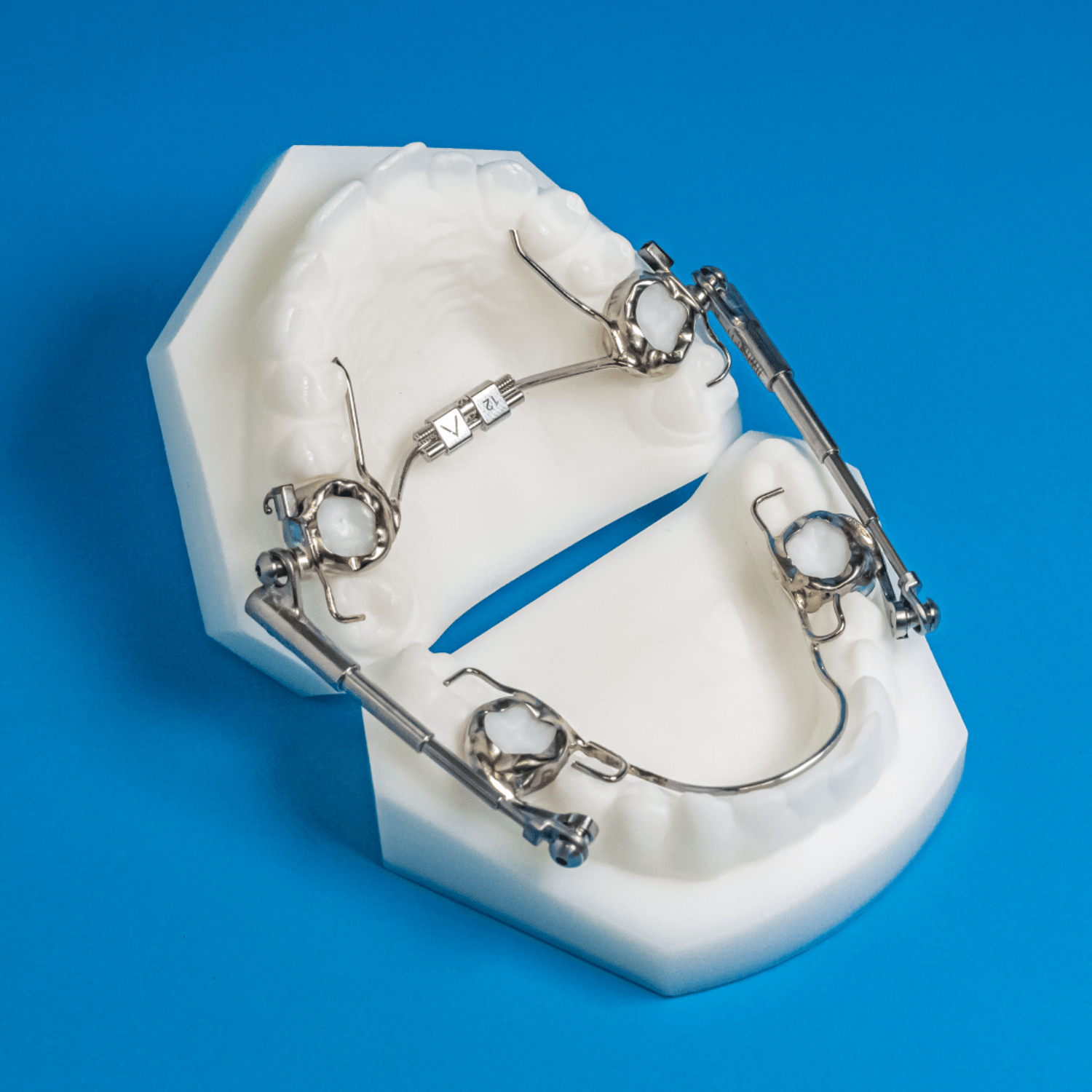
The MiniScope® Herbst we developed miniaturizes the telescoping rod-and-tube assembly to reduce buccal-corridor bulk while maintaining the bite-jumping mechanics. The smaller arms cut soft-tissue irritation and improve patient hygiene access without changing the underlying Class II correction protocol.
Lab-Side Observations on Herbst Failure Modes
What the lab sees when a Herbst case calls for repair tells a more specific story than the percentage averages.
The most common failure modes we field at the lab fall into a small set: attachment loosening (the appliance comes detached from the crown or band), telescope rod distortion or fracture (mechanical failure of the telescoping arm), L-pin or screw fractures (mechanical failure of the connection hardware), and cement or bond failures (anchorage loss at the tooth interface). Each is design-dependent. Each is also patient-dependent: heavy bruxers stress the mechanism differently than non-bruxers; lateral mandibular function patterns affect telescope wear; oral hygiene affects the cement-tooth interface durability.
For practitioners managing high Herbst caseloads, the conversation worth having with the lab is design-specific. If breakage is concentrated in attachment loosening, crown-mounted designs reduce that. If breakage is in the telescoping arms, mechanism choice matters. If breakage clusters around hygiene-related anchorage failures, the conversation is partly clinical (patient selection, hygiene reinforcement) and partly design (smaller, more cleansable hardware).
If a specific case is high-risk for Herbst breakage (heavy bruxer, poor hygiene history, atypical oral anatomy), call our tech team for case-design questions before submitting the prescription. A 10-minute design conversation prevents repair visits later.
When Each Herbst Design Fits
For straightforward Class II Division 1 cases in growing patients near the pubertal peak, most modern Herbst designs work. The choice is partly clinical preference and partly lab manufacturing capability.
For cases with hygiene concerns or soft-tissue sensitivity, miniaturized designs (MiniScope® family, modern compact telescoping mechanisms) reduce the buccal-corridor footprint and improve tolerance.
For heavy bruxers or cases at risk for mechanical breakage, crown-mounted designs and modern telescoping mechanisms reduce attachment failures.
For adult cases, the appliance still works, but the clinician should expect more dental and less skeletal effect, and should plan retention accordingly. Refer to our pillar reference on the Herbst for the Pancherz body of work on Herbst skeletal vs dental effect by patient age.
For cases where a different appliance category serves better, the MARA appliance is the most common alternative: different biomechanical approach, no telescoping arms, smaller buccal-corridor footprint, different breakage profile.
Frequently Asked Questions
How often does a Herbst appliance break?
Modern Herbst designs report complication rates in the 20-30% range over a full treatment course, with most complications being minor and chairside-repairable. Older banded designs reported rates as high as 88% in some published cohorts. The exact rate depends on appliance design, patient compliance with care instructions, and chewing patterns.
Does the Herbst appliance hurt?
Patients typically report soreness during the first 24-72 hours after delivery as the mandible adapts to the forward-held position, with discomfort decreasing as adaptation progresses.
Will my Herbst case relapse?
Some degree of relapse is common after Herbst treatment, though the magnitude varies. Pancherz’s long-term follow-up studies documented partial relapse in both the skeletal and dental components of Class II correction over the years following appliance removal. The relapse pattern depends on several factors: whether the Class II correction was achieved primarily through skeletal change (more stable in growing patients with continued mandibular growth) or through dental change (less stable without effective retention); the quality of retention protocol used post-Herbst; and the patient’s continued growth pattern.
Effective retention planning is more important for long-term Herbst case stability than initial Class II correction magnitude. For cases relying heavily on dental Class II correction (typical in non-growing or older adolescent patients), bonded or removable retention should be considered. For cases with strong skeletal response, retention requirements may be less intensive.
Relapse is the under-discussed clinical reality of Class II functional appliance treatment in general, not a Herbst-specific limitation. The same considerations apply to twin-block, bionator, and most other Class II correction strategies.
Can I prescribe a Herbst for an adult patient?
Yes, with caveats. Adult Herbst treatment is well-documented; Ruf and Pancherz (2006) reported successful Class I outcomes in 23 consecutive adult Class II Division 1 cases with pretreatment ages from 15.7 to 44.4 years. The skeletal response diminishes past the growth peak, so adult Herbst cases rely more heavily on dentoalveolar effect. Adult patients should be informed that the Class II correction will be primarily dental rather than skeletal, and that retention is critical to long-term stability.
Conclusion
The Herbst appliance is a mature, well-documented Class II correction option with clear advantages (built-in compliance, predictable timeline, robust skeletal response in growing patients) and real, design-dependent disadvantages (breakage rates that vary widely by design, hygiene burden, post-treatment relapse risk). The prescription decision benefits from reading the trade-offs by design parameter rather than by appliance category.
If a specific case is borderline, submit the scan for case-design review before prescribing the appliance.